As yoga teachers, we often work with students who are managing high blood pressure, sometimes knowingly and sometimes not. Because hypertension usually has no symptoms, it can go unnoticed for years, silently raising the risk of heart attack, stroke, and kidney disease. Understanding how yoga can influence blood pressure allows us to teach with clarity, sensitivity, and confidence, grounded in physiology rather than fear.
The question isn’t simply whether yoga “lowers” blood pressure, but how it might support the body’s intricate systems that regulate it.
👉Understanding Blood Pressure
Blood pressure (BP) is the force of blood against the walls of the arteries as the heart contracts and relaxes. It’s expressed as two numbers: systolic pressure (the peak pressure when the heart beats) over diastolic pressure (the resting pressure between beats). A typical healthy reading is below 120/80 mm Hg.
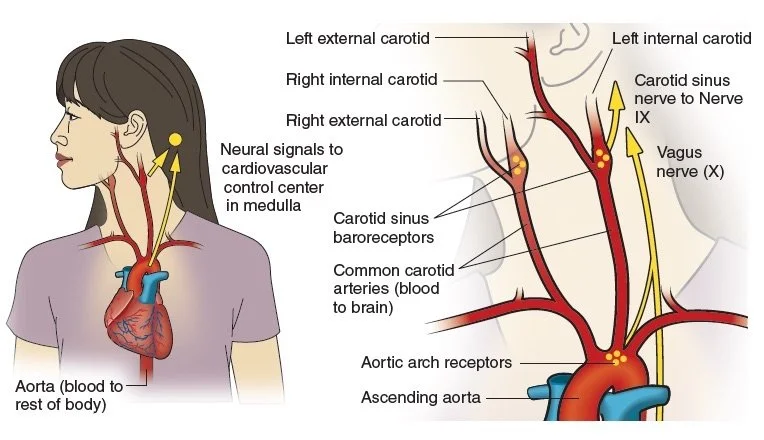
Our bodies maintain BP through a remarkable feedback system called the baroreceptor reflex. These pressure-sensitive receptors, located in the carotid sinuses of the neck and the aortic arch, detect changes in vessel stretch and send messages to the autonomic nervous system via the glossopharyngeal and vagus nerves (Al-Khazraji & Shoemaker 2018). When BP drops, the sympathetic branch increases heart rate and constricts blood vessels; when BP rises, the opposite occurs.
This constant fine-tuning allows blood flow to match the body’s needs, whether during a sprint, a yoga class, or a moment of deep rest.
👉Hypertension: A Common Challenge
Hypertension (persistently high BP) is a global health issue. Around one in three adults is affected (Kearney et al. 2005). Most cases are essential hypertension, meaning no single cause is identifiable (Messerli, Williams & Ritz 2007). However, contributing factors include:
Excess salt intake (Meneton et al. 2005)
Obesity and insulin resistance
Sedentary lifestyle and emotional stress
Ageing and low potassium intake (Takahashi et al. 2011)
The most recent international guidelines define hypertension as ≥130/80 mm Hg in adults (Whelton et al. 2018). Maintaining levels below this significantly reduces the risk of cardiovascular events.
👉What the Research Says About Yoga and Blood Pressure
A systematic review and meta-analysis found that yoga can be preliminarily recommended as an effective intervention for reducing BP (Hagins et al. 2013). However, the authors cautioned that many studies were small, lacked randomisation, or poorly described the yoga interventions.
Despite these limitations, several mechanisms have been proposed:
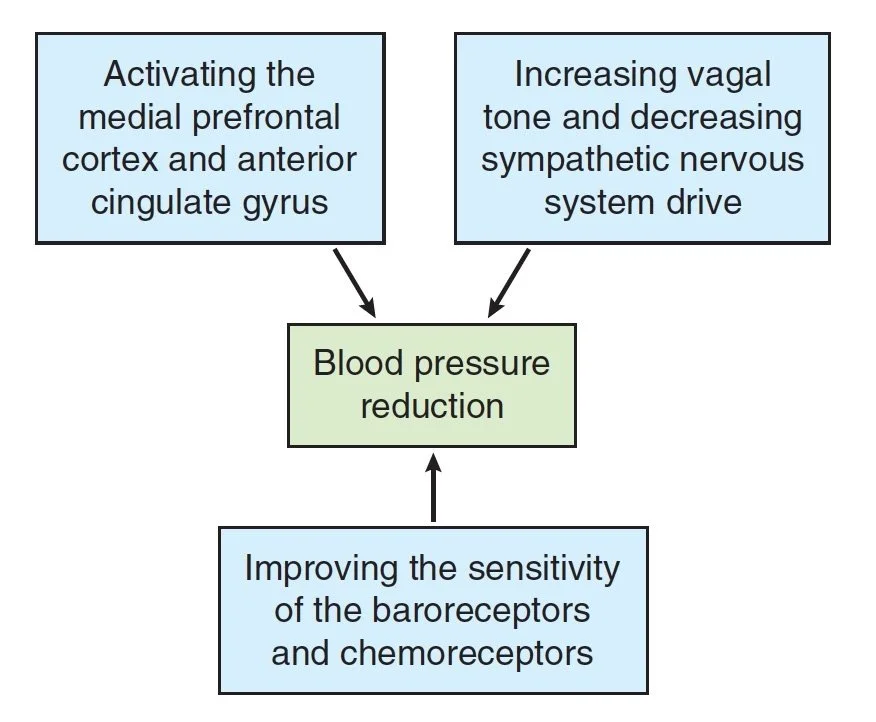
Enhanced baroreceptor sensitivity – Regular yoga practice may help the body detect and respond to changes in BP more efficiently (Selvamurthy et al. 1998).
Improved autonomic balance – Yoga appears to reduce sympathetic nervous system activity (the ‘fight-or-flight’ response) and increase parasympathetic (vagal) tone, promoting cardiovascular calm (Vijayalakshmi et al. 2004).
Slow breathing effects – Controlled breathing, a hallmark of yoga, has been shown to improve baroreflex sensitivity and lower BP in people with essential hypertension (Bernardi et al. 2001; Joseph et al. 2005).
Meditation and attention training – Focused awareness activates brain regions such as the medial prefrontal cortex and anterior cingulate gyrus, both involved in regulating BP and emotional stress (Posner & Petersen 1990; Williamson, McColl & Mathews 2004).
The takeaway is that it’s the state yoga creates, including mindful attention, slower breathing, and reduced reactivity, that seems most beneficial for cardiovascular health, not specific poses alone.
👉Teaching Yoga to Students with Hypertension
When teaching students with hypertension, a few clear principles can help create safety, inclusivity, and empowerment.
1. Confirm medical clearance.
Students with uncontrolled hypertension should seek approval from a healthcare professional before joining class. Controlled hypertension generally does not require significant restrictions.
2. Modify inversions.
Elevating the legs and heart above the head can increase BP temporarily. Avoid full inversions such as Shoulder Stand (Salamba Sarvangasana) and Headstand (Sirsasana).
Partial inversions like Downward Facing Dog (Adho Mukha Svanasana) can be practised with modifications such as hands on blocks or a chair to reduce pressure in the head.
3. Choose calming rather than stimulating practices.
Emphasise slow, mindful movement, gentle breathwork, and longer relaxation periods. Avoid strong breath retentions or fast, forceful pranayama such as Kapalabhati or Bhastrika.
4. Prioritise the parasympathetic response.
Invite restorative postures, supported forward folds, and supine relaxation to downregulate the nervous system. The restorative effects of yoga, rather than intensity or exertion, appear most beneficial for BP regulation.
5. Encourage self-awareness and agency.
Students should feel empowered to come out of postures, adjust props, or rest at any time. Language such as “notice what feels steady” or “choose the version that helps you breathe comfortably” promotes autonomy.
6. Educate gently.
Understanding the physiological ‘why’ helps students practise intelligently. Explain that yoga may support cardiovascular regulation by improving the body’s internal sensitivity, not by “curing” hypertension.
[Insert “McGonigle-IG-quote-template” image]
👉Looking Ahead
While yoga shows promise for managing blood pressure, its most valuable contribution may be less about numbers and more about nervous system resilience. As teachers, when we help students cultivate awareness, steady breathing, and calm attention, we are influencing the very systems that help regulate the heart and vessels.
The art of teaching yoga for hypertension lies in balancing science and sensitivity—guiding students toward calm without instilling fear.
References:
Al-Khazraji, B., and J. Shoemaker. 2018. “The Human Cortical Autonomic Network and Volitional Exercise in Health and Disease.” Applied Physiology, Nutrition, and Metabolism 43 (11): 1122-1130.
Bernardia, L., A. Gabuttia, C. Portaa, and L. Spicuzza. 2001. “Slow Breathing Reduces Chemoreflex Response to Hypoxia and Hypercapnia and Increases Baroreflex Sensitivity.” Journal of Hypertension 19:2221-2229.
Cole, R. 1989. “Postural Baroreflex Stimuli May Affect EEG Arousal and Sleep in Humans.” Journal of Applied Physiology 67 (6): 2369-2375.
Hagins, M., R. States, T. Selfe, and K. Innes. 2013. “Effectiveness of Yoga for Hypertension: Systematic Review and Meta-Analysis.” Evidence-Based Complementary and Alternative Medicine 2013: 649836.
Joseph, C., C. Porta, G. Casucci, N. Casiraghi, M. Maffeis, M. Rossi, and L. Bernardi. 2005. “Slow Breathing Improves Arterial Baroreflex Sensitivity and Decreases Blood Pressure in Essential Hypertension.” Hypertension 46 (4): 714-718.
Kearney, P., M. Whelton, K. Reynolds, P. Muntner, P. Whelton, and J. He. 2005. “Global Burden of Hypertension: Analysis of Worldwide Data.” Lancet 365 (9455): 217-223.
Meneton, P., X. Jeunemaitre, H. de Wardener, and G. MacGregor. 2005. “Links Between Dietary Salt Intake, Renal Salt Handling, Blood Pressure, and Cardiovascular Diseases.” Physiology Reviews 85 (2): 679-715.
Messerli, F., B. Williams, and E. Ritz. 2007. “Essential Hypertension.” Lancet 370 (9587): 591-603.
Posner, M., and S. Petersen. 1990. “The Attention System of the Human Brain.” Annual Review of Neuroscience 13:25-42.
Razin, A. 1977. “Upside-Down Position to Terminate Tachycardia of Wolff-Parkinson-White Syndrome.” New England Journal of Medicine 296 (26): 1535‐1536.
Schneider, R., F. Staggers, C. Alexander, W. Sheppard, M. Rainforth, K. Kondwani, S. Smith, and C. King. 1995. “A Randomised Controlled Trial of Stress Reduction for Hypertension in Older African Americans.” Hypertension 26 (5): 820-857.
Selvamurthy, W., K. Sridharan, U. Ray, R. Tiwary, K. Hegde, U. Radhakrishan, and K. Sinha. 1998. “A New Physiological Approach to Control Essential Hypertension.” Indian Journal of Physiology and Pharmacology 42 (2): 205-213.
Tai, Y., and C. Colaco. 1981. “Upside-Down Position for Paroxysmal Supraventricular Tachycardia.” Lancet 2 (8258): 1289.
Takahashi, H., M. Yoshika, Y. Komiyama, and M. Nishimura. 2011. “The Central Mechanism Underlying Hypertension: A Review of the Roles of Sodium Ions, Epithelial Sodium Channels, the Renin-Angiotensin-Aldosterone System, Oxidative Stress and Endogenous Digitalis in the Brain.” Hypertension Research 34 (11): 1147-1160.
Vijayalakshmi, P., Madanmohan, A.B. Bhavanani, A. Patil, and K. Babu. 2004. “Modulation of Stress Induced by Isometric Handgrip Test in Hypertensive Patients Following Yogic Relaxation Training.” Indian Journal of Physiology and Pharmacology 48:59-64.
Whelton, P., R. Carey, W. Aronow, D. Casey, K. Collins, C. Dennison Himmelfarb, S. DePalma, S. Gidding, K. Jamerson, D. Jones, et al. 2018. “2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults.” Journal of the American College of Cardiology 71 (19): e127-e248.
Williamson, J., R. McColl, and D. Mathews. 2004. “Changes in Regional Cerebral Blood Flow Distribution During Postexercise Hypotension in Humans.” Journal of Applied Physiology 96 (2): 719-724.